After pregnancy, many women look forward to bonding with their newborn and settling into a new routine. For people living with migraine, however, the postpartum period can feel especially challenging. Hormonal changes, sleep deprivation, skipped meals, and stress can all increase the risk of migraine attacks. At the same time, breastfeeding mothers often worry about whether migraine medications could harm their baby.
The good news is that migraine and breastfeeding are not mutually exclusive. With thoughtful planning and evidence-based guidance, it is possible to treat migraine effectively while protecting your infant. Understanding which treatments are considered safe can help you feel more confident and supported during this stage of life.
Migraine in the Postpartum Period
Many women notice that migraine patterns change after delivery. Some experience a welcome break during pregnancy, only to have attacks return weeks later. Others see little change at all.
A common pattern is the return of migraine within the first month postpartum. Estrogen levels drop rapidly after delivery, which can trigger attacks in people who are hormonally sensitive. Sleep disruption is another major factor. Newborn care often means frequent night awakenings, irregular schedules, and physical exhaustion, all of which are well-known migraine triggers.
Breastfeeding itself affects migraine differently from person to person. Some women report fewer attacks while nursing, possibly due to more stable hormone levels compared to formula feeding. Others notice no improvement or even worsening symptoms. There is no single “normal” experience, which is why individualized treatment matters so much.
General Principles of Migraine Treatment While Breastfeeding
When managing migraine during breastfeeding, most clinicians follow a few core principles. These guidelines help balance symptom relief with infant safety.
Using the lowest effective dose for the shortest necessary time reduces medication exposure through breast milk. Drugs with established safety records in lactation are preferred whenever possible. Timing also matters. Taking medication immediately after breastfeeding or pumping can allow drug levels in milk to decline before the next feed.
Non-drug strategies remain the foundation of migraine care in the postpartum period. Regular meals, adequate hydration, short naps when possible, and gentle stress reduction can significantly reduce attack frequency. These lifestyle measures may feel simple, but they are powerful tools when used consistently.
Acute Migraine Treatment Options While Breastfeeding
Acute treatments are used to stop migraine attacks once they start. Several commonly used options are considered compatible with breastfeeding.
Acetaminophen is widely regarded as safe and is often the first-line choice for mild to moderate migraine attacks. It passes into breast milk in very small amounts and has a long history of use in nursing mothers.
Nonsteroidal anti-inflammatory drugs, or NSAIDs, are also commonly used. Ibuprofen is considered especially safe during breastfeeding due to its short half-life and minimal transfer into breast milk. Naproxen is generally compatible as well when used occasionally. Aspirin, however, is usually avoided in breastfeeding because of concerns about Reye’s syndrome in infants.
Triptans are often essential for moderate to severe migraine. Sumatriptan is the most studied triptan in breastfeeding and is considered safe. Only tiny amounts enter breast milk, and absorption by the infant is minimal. Other triptans have less published data, but available evidence suggests low risk. Some mothers choose to pump and discard milk for several hours after taking a triptan, but most professional guidelines state this step is not necessary.
Migraine-related nausea can be just as disabling as head pain. Several anti-nausea medications are considered safe during breastfeeding. Metoclopramide and domperidone have been used extensively and may even increase milk supply by raising prolactin levels. Ondansetron is also considered compatible with breastfeeding and is commonly prescribed.
Preventive Migraine Treatments During Breastfeeding
Preventive medications are taken regularly to reduce how often migraine attacks occur. Many breastfeeding mothers prefer to avoid daily medications, but some need them due to frequent or severe migraine.
Certain beta-blockers are commonly used preventives in the postpartum period. Propranolol and metoprolol are generally considered safe during breastfeeding. Infants should be monitored for signs of low heart rate or unusual sleepiness, but serious problems are rare.
Amitriptyline is another preventive option with reassuring safety data. Levels in breast milk are low, and it is often used when migraine is accompanied by sleep problems or mood symptoms.
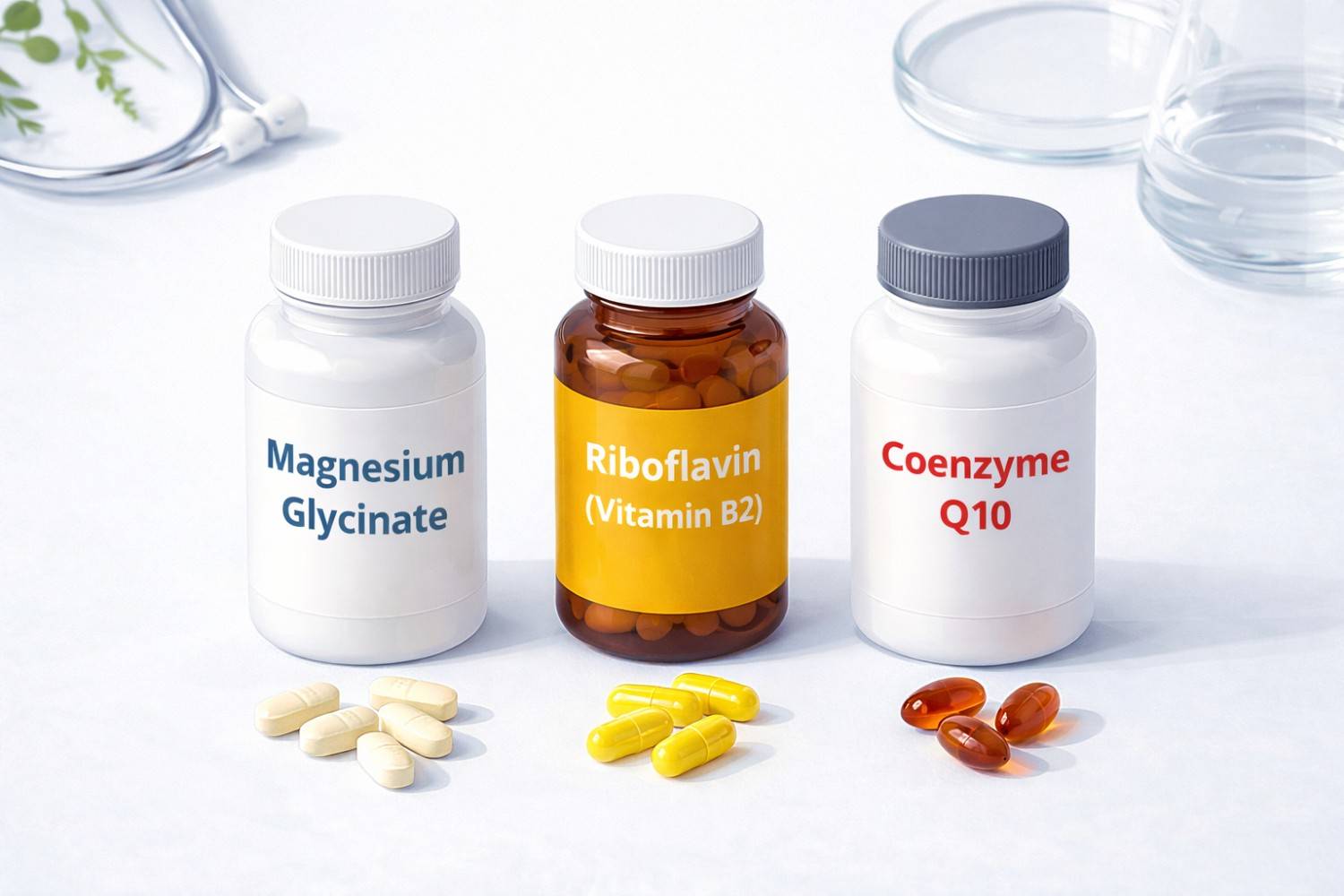
Non-drug preventives are especially appealing during breastfeeding. Magnesium and riboflavin (vitamin B2) are both considered safe and may reduce migraine frequency for some people. These supplements are often recommended as first steps before starting prescription preventives.
Newer migraine treatments, such as CGRP monoclonal antibodies, have very limited data in breastfeeding. Because of this uncertainty, they are usually avoided until more research is available. Topiramate does pass into breast milk in small amounts. Some guidelines allow cautious use, but infant growth and development should be monitored closely.
Migraine Treatments to Avoid or Use With Caution
Not all migraine treatments are compatible with breastfeeding. Valproate is generally contraindicated because of risks to infant liver health and development. Ergot derivatives are unsafe due to strong blood vessel constriction and their potential to reduce milk supply.
Aspirin is also discouraged in breastfeeding, especially at higher doses, because of the theoretical risk of Reye’s syndrome. When in doubt, it is always best to check a reliable reference or speak directly with a healthcare professional.
Practical Strategies for Breastfeeding Mothers With Migraine
Small adjustments can make a meaningful difference in managing migraine while breastfeeding. Timing medication doses right after feeds can help minimize infant exposure. Keeping a close eye on both mother and baby is important when preventive medications are used. Watch for unusual infant sleepiness, feeding difficulties, or irritability, and report concerns promptly.
Hydration and nutrition are especially important in the postpartum period. Skipped meals and dehydration are common migraine triggers when caring for a newborn. Simple snacks, water bottles within reach, and gentle reminders can help maintain consistency.
Support systems matter. Sharing nighttime feedings with a partner when possible or accepting help from family members can reduce sleep deprivation, one of the strongest migraine triggers. Reliable information sources are also essential. LactMed, maintained by the U.S. National Library of Medicine, provides up-to-date evidence on medication safety during breastfeeding and is trusted by clinicians worldwide. You can access it here: https://www.ncbi.nlm.nih.gov/books/NBK501922/
For broader migraine guidance, authoritative resources include the American Migraine Foundation (https://americanmigrainefoundation.org/) and peer-reviewed research published in journals such as Neurology and Headache: The Journal of Head and Face Pain.
Take-Home Message
Migraine management during breastfeeding is not only possible, it is often very effective with the right approach. Acute treatments such as acetaminophen, ibuprofen, naproxen, sumatriptan, and several anti-nausea medications are considered safe for nursing mothers. Preventive options like propranolol, metoprolol, and amitriptyline can be used when needed, while supplements such as magnesium and riboflavin offer non-drug support.
Every mother’s situation is unique. With careful medication selection, smart timing, and guidance from a healthcare provider familiar with migraine and lactation, it is possible to control migraine attacks while continuing to breastfeed confidently.
This content is for informational purposes only and does not replace medical advice. Always consult your healthcare provider before starting or changing migraine treatments while breastfeeding.