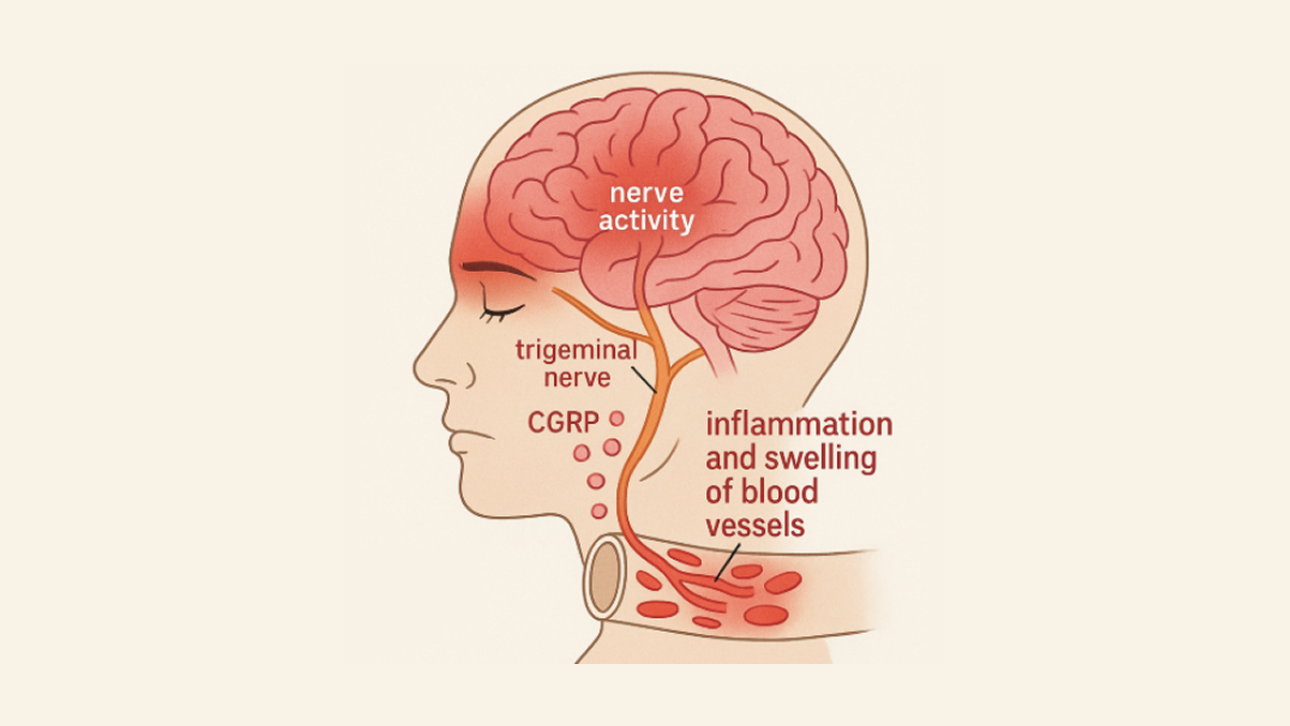
Living with migraine can feel like navigating a storm with no clear path home. But science is on your side. While CGRP blockers changed migraine care a decade ago, a new target is emerging: PACAP.
PACAP is reshaping how we think about preventing and stopping attacks. In this post, we’ll break down the latest research, practical tips, and what this means for you.
What Is PACAP and Why It Matters
PACAP (pituitary adenylate cyclase-activating peptide) is a small protein in the brain. It helps regulate blood flow, pain signals, and inflammation. Studies show that PACAP levels rise during migraine attacks.
In fact:
In healthy volunteers, an intravenous infusion of PACAP triggered migraine-like headaches. [1]
Patients often experience photophobia and throbbing pain similar to typical migraine.
Blocking PACAP or its receptors could cut down migraine days and reduce severity. That’s why researchers now view PACAP migraine treatment as a top next-generation target.
New Therapies on the Horizon
Pharmaceutical labs are racing to develop monoclonal antibodies against PACAP or its receptor.
Early-stage trials offer hope:
• Clinical Trials: Phase 2 studies report a 30%–40% drop in monthly migraine days so far. [2]
• Safety Profile: Researchers are assessing long-term effects, since PACAP is involved in heart function and digestion.
• Comparison to CGRP: PACAP and CGRP pathways overlap but remain distinct. If CGRP blockers didn’t work for you, PACAP migraine treatment might.
Beyond PACAP: Other Promising Targets
PACAP isn’t the only new player. Here are three more areas under investigation:
1. KATP Channels
These potassium channels help control blood vessel dilation. Early research suggests that blocking KATP channels can abort an attack. Check out this study in Headache: The Journal of Head and Face Pain. [3]
2. Glutamate Modulation
Glutamate drives nerve cell communication and may underlie aura and central sensitization. Drugs that dampen glutamate signaling are in early trials. The Neurology Journal reports promising animal data. [4]
3. Orexin System
Orexins regulate sleep and arousal. Since poor sleep triggers migraines, orexin receptor blockers are being tested for both insomnia and headache prevention.
4. Personalized Medicine
Genome-wide studies in JAMA reveal gene variants tied to migraine risk. One day, your care plan might match your DNA, unlocking truly personalized PACAP migraine treatment strategies.
Devices and Digital Health: Non-Drug Allies
Medications aren’t the only tools in the migraine toolbox. Advances in neuromodulation and digital care are gaining traction.
- Wearable Nerve Stimulators: New trigeminal and vagus nerve devices offer on-demand relief. Learn more from this article in The Lancet. [5]
- Remote Electrical Neuromodulation (REN): Compact gadgets you control via smartphone apps. They send gentle pulses to halt an attack.
- Digital Therapeutics: Migrainers swear by smartphone-based CBT, biofeedback, and mindfulness apps. These tools boost resilience and help you track triggers.
Practical Tips While You Wait
While PACAP migraine treatment trials progress, here’s what you can do now:
1. Stay Informed
Ask your neurologist about local PACAP trials or registries. ClinicalTrials.gov is a good starting point.
2. Track Your Response
Use a headache diary app. Record frequency, intensity, and triggers. This data guides your doctor and pinpoints if a new therapy is right for you.
3. Advocate for Access
New drugs often carry high price tags. Reach out to patient advocacy groups for support. They can help with insurance appeals.
4. Combine Strategies
Don’t rely on pills alone. Add stress management, regular sleep, hydration, and gentle exercise.
Frequently Asked Questions
Q: How soon will PACAP treatments be available?
A: If phase 3 trials go well, we could see FDA approval in 2–3 years.
Q: Are there risks to blocking PACAP?
A: Potential side effects include mild digestive issues or changes in blood pressure. Long-term safety data is still pending.
Q: Should I stop my current migraine meds?
A: Never stop or change prescriptions without talking to your doctor. Combining therapies may yield the best results.
The Future of Migraine Care
The migraine landscape is evolving fast. PACAP migraine treatment sits at the cutting edge, offering hope to people who haven’t found relief yet. As research unfolds, expect a more personalized approach that blends:
- Targeted medications like PACAP or CGRP antibodies
- Neuromodulation devices for on-the-spot relief
- Digital tools for stress and trigger management
- Lifestyle tweaks based on genetics and personal patterns
You’re not alone in this journey. With new options on the horizon, better days lie ahead.
References
[1] Schytz HW, et al. Cephalalgia. 2009;29(7):861–873. https://doi.org/10.1111/j.1468-2982.2008.01840.x
[2] The Lancet Neurology. Early Phase 2 PACAP Antibody Trial Results. 2023. https://www.thelancet.com/journals/laneur/article/PIIS1474-4422(23)00012-3/fulltext
[3] Headache: The Journal of Head and Face Pain, 2021;61(2):223–232. https://headachejournal.onlinelibrary.wiley.com/doi/10.1111/head.14056
[4] Neurology Journal. Glutamate Modulators in Migraine Prevention. 2022. https://n.neurology.org/content/98/12/567
[5] The Lancet. Wearable Nerve Stimulation for Migraine. 2022. https://www.thelancet.com/journals/lanres/article/PIIS2213-2600(21)00045-7/fulltext