For people living with chronic migraine—defined as 15 or more headache days per month, with at least 8 migraine days—the burden can be profound. Work, family life, and mental health often suffer, and relying on acute medications alone is rarely enough.
One of the most effective and well-studied preventive treatments for chronic migraine is onabotulinumtoxinA, better known by the brand name Botox. Unlike many older preventives, Botox is specifically approved for chronic migraine and has a strong evidence base supporting long-term use.
How Botox Works in Migraine
Botox is a purified neurotoxin derived from Clostridium botulinum. When injected in very small amounts into specific muscles of the head and neck, it does not work the same way as cosmetic Botox.
In migraine prevention, Botox:
- Blocks the release of pain-related neurotransmitters such as CGRP and substance P
- Calms overactive pain pathways in the trigeminal nerve system
- Reduces peripheral nerve sensitization, making migraine attacks less likely to start
Rather than relaxing muscles alone, Botox primarily acts on pain signaling, helping prevent migraine before it escalates.
Evidence for Effectiveness
The strongest evidence for Botox comes from the landmark PREEMPT 1 and PREEMPT 2 trials, which established Botox as an effective preventive therapy for chronic migraine.
These large randomized studies showed that Botox:
- Reduced monthly headache days by an average of 8–9 days
- Significantly improved quality-of-life and disability scores
- Became more effective with repeated treatment cycles, highlighting the importance of consistency
Results from these trials were published in leading journals such as Headache: The Journal of Head and Face Pain and Neurology.
You can explore these findings further here:
https://headachejournal.onlinelibrary.wiley.com
https://www.neurology.org
Real-world clinical experience has confirmed these results, with many patients reporting fewer, shorter, and less severe migraine attacks after several rounds of treatment.
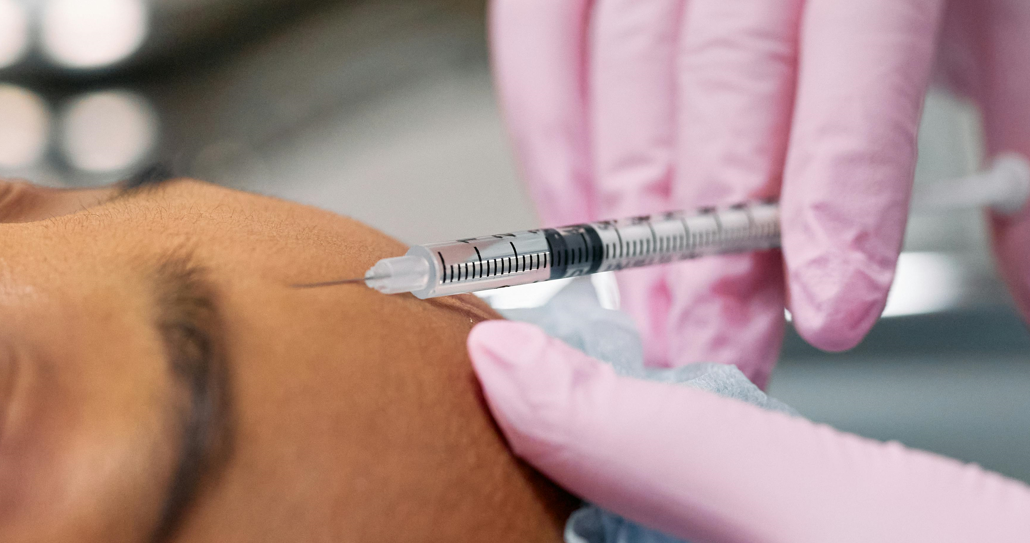
The Botox Procedure for Chronic Migraine
Botox is administered every 12 weeks in a neurologist’s or headache specialist’s office.
What to expect:
- Injection pattern: Approximately 31 injections across the forehead, temples, scalp, back of the head, neck, and shoulders
- Time required: About 10–15 minutes
- Anesthesia: Not required; needles are very small and discomfort is brief
Although the number of injections may sound intimidating, most patients tolerate the procedure well and describe it as manageable.
Side Effects and Safety
Botox is generally well tolerated, especially when administered by an experienced provider.
Common side effects include:
- Neck pain or stiffness
- Local soreness at injection sites
- Mild shoulder or neck weakness
Less common:
- Eyelid drooping (ptosis)
- Temporary changes in neck posture
These effects are usually mild and resolve within days to weeks. Serious side effects are rare when proper dosing and injection techniques are used.
Importantly, Botox does not cause weight gain, sedation, or cognitive side effects, which makes it appealing for long-term use.
Who Is a Candidate for Botox?
Botox is approved only for chronic migraine, not episodic migraine.
To qualify, patients typically must:
- Have 15 or more headache days per month, with at least 8 migraine days, for at least 3 months
- Have other causes of frequent headache ruled out
- Have tried and failed at least two oral preventive medications, unless contraindicated or poorly tolerated
Eligibility requirements may vary slightly depending on insurance or provincial coverage policies.
How Soon Does Botox Start Working?
Response timing varies:
- Some patients notice improvement after the first treatment cycle
- Most require 2–3 cycles (6–9 months) to fully assess benefit
If no meaningful improvement is seen after three treatment cycles, Botox is usually discontinued and alternative options are explored.
Access and Coverage in Canada
Botox for chronic migraine is often covered in Canada, though approval usually requires documentation.
Coverage pathways include:
- Provincial drug programs, once eligibility criteria and prior authorization are met
- Private insurance plans, with proof of chronic migraine diagnosis and preventive treatment failures
- Hospital-based programs in some regions, where treatment costs may be partially or fully supported
Neurologists and headache clinics are typically familiar with the approval process and required paperwork.
Practical Tips for Patients
- Keep a headache diary to document headache days and treatment response
- Plan ahead, as injections are required every 12 weeks
- Be patient, since benefits often build over multiple cycles
- Report side effects, especially neck weakness or eyelid drooping
- Combine Botox with lifestyle strategies, such as regular sleep, stress management, and trigger reduction
Many patients also use Botox alongside other preventives, including CGRP monoclonal antibodies, when appropriate.
Take-Home Message
Botox is a proven, effective preventive treatment for chronic migraine. By calming pain pathways in the head and neck, it significantly reduces headache frequency, improves quality of life, and offers relief to patients whose migraines are otherwise difficult to control.
Although it requires ongoing injections every three months, many people find the benefits far outweigh the inconvenience. For eligible patients with chronic migraine, Botox can be a transformative part of long-term migraine management.